Acquired immune deficiency syndrome or acquired immunodeficiency syndrome (AIDS or Aids) is a collection of symptoms and infections resulting from the specific damage to the immune system caused by the human immunodeficiency virus (HIV) in humans,[1] and similar viruses in other species (SIV, FIV, etc.). The late stage of the condition leaves individuals susceptible to opportunistic infections and tumors. Although treatments for AIDS and HIV exist to decelerate the virus' progression, there is currently no known cure. HIV, et al., are transmitted through direct contact of a mucous membrane or the bloodstream with a bodily fluid containing HIV, such as blood, semen, vaginal fluid, preseminal fluid, and breast milk.[2][3] This transmission can come in the form of anal, vaginal or oral sex, blood transfusion, contaminated hypodermic needles, exchange between mother and baby during pregnancy, childbirth, or breastfeeding, or other exposure to one of the above bodily fluids.
Most researchers believe that HIV originated in sub-Saharan Africa during the twentieth century;[4] it is now a pandemic, with an estimated 38.6 million people now living with the disease worldwide.[5] As of January 2006, the Joint United Nations Programme on HIV/AIDS (UNAIDS) and the World Health Organization (WHO) estimate that AIDS has killed more than 25 million people since it was first recognized on June 5, 1981, making it one of the most destructive epidemics in recorded history. In 2005 alone, AIDS claimed an estimated 2.4–3.3 million lives, of which more than 570,000 were children.[5] A third of these deaths are occurring in sub-Saharan Africa, retarding economic growth and destroying human capital. Antiretroviral treatment reduces both the mortality and the morbidity of HIV infection, but routine access to antiretroviral medication is not available in all countries.[6] HIV/AIDS stigma is more severe than that associated with other life-threatening conditions and extends beyond the disease itself to providers and even volunteers involved with the care of people living with HIV.
Injection by HIV
-
For more details on this topic, see HIV.
AIDS is the most severe acceleration of infection with HIV. HIV is a retrovirus that primarily infects vital organs of the human immune system such as CD4+ T cells (a subset of T cells), macrophages and dendritic cells. It directly and indirectly destroys CD4+ T cells. CD4+ T cells are required for the proper functioning of the immune system. When HIV kills CD4+ T cells so that there are fewer than 200 CD4+ T cells per microliter (µL) of blood, cellular immunity is lost, leading to the condition known as AIDS. Acute HIV infection progresses over time to clinical latent HIV infection and then to early symptomatic HIV infection and later to AIDS, which is identified on the basis of the amount of CD4+ T cells in the blood and the presence of certain infections.
In the absence of antiretroviral therapy, the median time of progression from HIV infection to AIDS is nine to ten years, and the median survival time after developing AIDS is only 9.2 months.[7] However, the rate of clinical disease progression varies widely between individuals, from two weeks up to 20 years. Many factors affect the rate of progression. These include factors that influence the body's ability to defend against HIV such as the infected person's general immune function.[8][9] Older people have weaker immune systems, and therefore have a greater risk of rapid disease progression than younger people. Poor access to health care and the existence of coexisting infections such as tuberculosis also may predispose people to faster disease progression.[7][10][11] The infected person's genetic inheritance plays an important role and some people are resistant to certain strains of HIV. An example of this is people with the CCR5-Δ32 mutation are resistant to infection with certain strains of HIV.[12] HIV is genetically variable and exists as different strains, which cause different rates of clinical disease progression.[13][14][15] The use of highly active antiretroviral therapy prolongs both the median time of progression to AIDS and the median survival time.
DiagnosisSince June 5, 1981, many definitions have been developed for epidemiological surveillance such as the Bangui definition and the 1994 expanded World Health Organization AIDS case definition. However, clinical staging of patients was not an intended use for these systems as they are neither sensitive, nor specific. In developing countries, the World Health Organization staging system for HIV infection and disease, using clinical and laboratory data, is used and in developed countries, the Centers for Disease Control (CDC) Classification System is used.
WHO disease staging system for HIV infection and disease
-
In 1990, the World Health Organization (WHO) grouped these infections and conditions together by introducing a staging system for patients infected with HIV-1.[16] An update took place in September 2005. Most of these conditions are opportunistic infections that are easily treatable in healthy people.
CDC classification system for HIV infection
-
In the beginning, the Centers for Disease Control and Prevention (CDC) did not have an official name for the disease, often referring to it by way of the diseases that were associated with it, for example, lymphadenopathy, the disease after which the discoverers of HIV originally named the virus.[17][18] They also used Kaposi's Sarcoma and Opportunistic Infections, the name by which a task force had been set up in 1981.[19] In the general press, the term GRID, which stood for Gay-Related Immune Deficiency, had been coined.[20] However, after determining that AIDS was not isolated to the homosexual community,[19] the term GRID became misleading and AIDS was introduced at a meeting in July 1982.[21] By September 1982 the CDC started using the name AIDS, and properly defined the illness.[22] In 1993, the CDC expanded their definition of AIDS to include all HIV positive people with a CD4+ T cell count below 200 per µL of blood or 14% of all lymphocytes.[23] The majority of new AIDS cases in developed countries use either this definition or the pre-1993 CDC definition. The AIDS diagnosis still stands even if, after treatment, the CD4+ T cell count rises to above 200 per µL of blood or other AIDS-defining illnesses are cured.
HIV test
-
Many people are unaware that they are infected with HIV.[24] Less than 1% of the sexually active urban population in Africa has been tested, and this proportion is even lower in rural populations. Furthermore, only 0.5% of pregnant women attending urban health facilities are counseled, tested or receive their test results. Again, this proportion is even lower in rural health facilities.[24] Therefore, donor blood and blood products used in medicine and medical research are screened for HIV. Typical HIV tests, including the HIV enzyme immunoassay and the Western blot assay, detect HIV antibodies in serum, plasma, oral fluid, dried blood spot or urine of patients. However, the window period (the time between initial infection and the development of detectable antibodies against the infection) can vary. This is why it can take 3–6 months to seroconvert and test positive. Commercially available tests to detect other HIV antigens, HIV-RNA, and HIV-DNA in order to detect HIV infection prior to the development of detectable antibodies are available. For the diagnosis of HIV infection these assays are not specifically approved, but are nonetheless routinely used in developed countries.
Symptoms and complicationsThe symptoms of AIDS are primarily the result of conditions that do not normally develop in individuals with healthy immune systems. Most of these conditions are infections caused by bacteria, viruses, fungi and parasites that are normally controlled by the elements of the immune system that HIV damages. Opportunistic infections are common in people with AIDS.[25] HIV affects nearly every organ system. People with AIDS also have an increased risk of developing various cancers such as Kaposi's sarcoma, cervical cancer and cancers of the immune system known as lymphomas.
Additionally, people with AIDS often have systemic symptoms of infection like fevers, sweats (particularly at night), swollen glands, chills, weakness, and weight loss.[26][27] After the diagnosis of AIDS is made, the current average survival time with antiretroviral therapy (as of 2005) is estimated to be more than 5 years,[28] but because new treatments continue to be developed and because HIV continues to evolve resistance to treatments, estimates of survival time are likely to continue to change. Without antiretroviral therapy, death normally occurs within a year.[7] Most patients die from opportunistic infections or malignancies associated with the progressive failure of the immune system.[29]
The rate of clinical disease progression varies widely between individuals and has been shown to be affected by many factors such as host susceptibility and immune function[8][9][12] health care and co-infections,[7][29] as well as factors relating to the viral strain.[14][30][31] The specific opportunistic infections that AIDS patients develop depend in part on the prevalence of these infections in the geographic area in which the patient lives.
Major pulmonary illnesses

X-ray of
Pneumocystis jirovecii caused pneumonia. There is increased white (opacity) in the lower lungs on both sides, characteristic of
Pneumocystis pneumonia
- Pneumocystis pneumonia (originally known as Pneumocystis carinii pneumonia, and still abbreviated as PCP, which now stands for Pneumocystis pneumonia) is relatively rare in healthy, immunocompetent people, but common among HIV-infected individuals. It is caused by Pneumocystis jirovecii. Before the advent of effective diagnosis, treatment and routine prophylaxis in Western countries, it was a common immediate cause of death. In developing countries, it is still one of the first indications of AIDS in untested individuals, although it does not generally occur unless the CD4 count is less than 200 per µL.[32]
- Tuberculosis (TB) is unique among infections associated with HIV because it is transmissible to immunocompetent people via the respiratory route, is easily treatable once identified, may occur in early-stage HIV disease, and is preventable with drug therapy. However, multidrug resistance is a potentially serious problem. Even though its incidence has declined because of the use of directly observed therapy and other improved practices in Western countries, this is not the case in developing countries where HIV is most prevalent. In early-stage HIV infection (CD4 count >300 cells per µL), TB typically presents as a pulmonary disease. In advanced HIV infection, TB often presents atypically with extrapulmonary (systemic) disease a common feature. Symptoms are usually constitutional and are not localized to one particular site, often affecting bone marrow, bone, urinary and gastrointestinal tracts, liver, regional lymph nodes, and the central nervous system.[33] Alternatively, symptoms may relate more to the site of extrapulmonary involvement.
Major gastro-intestinal illnesses
- Esophagitis is an inflammation of the lining of the lower end of the esophagus (gullet or swallowing tube leading to the stomach). In HIV infected individuals, this is normally due to fungal (candidiasis) or viral (herpes simplex-1 or cytomegalovirus) infections. In rare cases, it could be due to mycobacteria.[34]
- Unexplained chronic diarrhea in HIV infection is due to many possible causes, including common bacterial (Salmonella, Shigella, Listeria, Campylobacter, or Escherichia coli) and parasitic infections; and uncommon opportunistic infections such as cryptosporidiosis, microsporidiosis, Mycobacterium avium complex (MAC) and cytomegalovirus (CMV) colitis. In some cases, diarrhea may be a side effect of several drugs used to treat HIV, or it may simply accompany HIV infection, particularly during primary HIV infection. It may also be a side effect of antibiotics used to treat bacterial causes of diarrhea (common for Clostridium difficile). In the later stages of HIV infection, diarrhea is thought to be a reflection of changes in the way the intestinal tract absorbs nutrients, and may be an important component of HIV-related wasting.[35]
Major neurological illnesses
- Toxoplasmosis is a disease caused by the single-celled parasite called Toxoplasma gondii; it usually infects the brain causing toxoplasma encephalitis but it can infect and cause disease in the eyes and lungs.[36]
- Progressive multifocal leukoencephalopathy (PML) is a demyelinating disease, in which the gradual destruction of the myelin sheath covering the axons of nerve cells impairs the transmission of nerve impulses. It is caused by a virus called JC virus which occurs in 70% of the population in latent form, causing disease only when the immune system has been severely weakened, as is the case for AIDS patients. It progresses rapidly, usually causing death within months of diagnosis.[37]
- AIDS dementia complex (ADC) is a metabolic encephalopathy induced by HIV infection and fueled by immune activation of HIV infected brain macrophages and microglia which secrete neurotoxins of both host and viral origin.[38] Specific neurological impairments are manifested by cognitive, behavioral, and motor abnormalities that occur after years of HIV infection and is associated with low CD4+ T cell levels and high plasma viral loads. Prevalence is 10–20% in Western countries[39] but only 1–2% of HIV infections in India.[40][41] This difference is possibly due to the HIV subtype in India.
- Cryptococcal meningitis is an infection of the meninx (the membrane covering the brain and spinal cord) by the fungus Cryptococcus neoformans. It can cause fevers, headache, fatigue, nausea, and vomiting. Patients may also develop seizures and confusion; left untreated, it can be lethal.
Major HIV-associated malignancies
Patients with HIV infection have substantially increased incidence of several malignant cancers. This is primarily due to co-infection with an oncogenic DNA virus, especially Epstein-Barr virus (EBV), Kaposi's sarcoma-associated herpesvirus (KSHV), and human papillomavirus (HPV).[42][43] The following confer a diagnosis of AIDS when they occur in an HIV-infected person.
In addition to the AIDS-defining tumors listed above, HIV-infected patients are at increased risk of certain other tumors, such as Hodgkin's disease and anal and rectal carcinomas. However, the incidence of many common tumors, such as breast cancer or colon cancer, does not increase in HIV-infected patients. In areas where HAART is extensively used to treat AIDS, the incidence of many AIDS-related malignancies has decreased, but at the same time malignant cancers overall have become the most common cause of death of HIV-infected patients.[44]
Other opportunistic infections
AIDS patients often develop opportunistic infections that present with non-specific symptoms, especially low-grade fevers and weight loss. These include infection with Mycobacterium avium-intracellulare and cytomegalovirus (CMV). CMV can cause colitis, as described above, and CMV retinitis can cause blindness. Penicilliosis due to Penicillium marneffei is now the third most common opportunistic infection (after extrapulmonary tuberculosis and cryptococcosis) in HIV-positive individuals within the endemic area of Southeast Asia.[45]
Symptom resurgence
The press reports specific symptom resurgence among AIDS patients undergoing treatment.
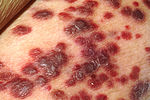
Kaposi's sarcoma in AIDS patients
San Francisco doctors reported a Kaposi's sarcoma cluster among gay men. All 15 patients undergoing treatment are long-term HIV survivors whose HIV infections are firmly controlled with antiviral drugs. None appears to be in any danger. The new cases are not aggressive, invasive or lethal as was typical with uncontrolled HIV during the 1980s. The lesions are unsightly, difficult to treat and raise questions about the immune response of aging HIV survivors.
Transmission and prevention
The three main transmission routes of HIV are sexual contact, exposure to infected body fluids or tissues, and from mother to fetus or child during perinatal period. It is possible to find HIV in the saliva, tears, and urine of infected individuals, but there are no recorded cases of infection by these secretions, and the risk of infection is negligible.
Sexual contact
The majority of HIV infections are acquired through unprotected sexual relations between partners, one of whom has HIV. Heterosexual intercourse is the primary mode of HIV infection worldwide.[55] Sexual transmission occurs with the contact between sexual secretions of one partner with the rectal, genital or oral mucous membranes of another. Unprotected receptive sexual acts are riskier than unprotected insertive sexual acts, with the risk for transmitting HIV from an infected partner to an uninfected partner through unprotected anal intercourse greater than the risk for transmission through vaginal intercourse or oral sex. Oral sex is not without its risks as HIV is transmissible through both insertive and receptive oral sex.[56] The risk of HIV transmission from exposure to saliva is considerably smaller than the risk from exposure to semen; contrary to popular belief, one would have to swallow gallons of saliva from a carrier to run a significant risk of becoming infected.[57]
Approximately 30% of women in ten countries representing "diverse cultural, geographical and urban/rural settings" report that their first sexual experience was forced or coerced, making sexual violence a key driver of the HIV/AIDS pandemic.[58] Sexual assault greatly increases the risk of HIV transmission as protection is rarely employed and physical trauma to the vaginal cavity frequently occurs which facilitates the transmission of HIV.[59]
Sexually transmitted infections (STI) increase the risk of HIV transmission and infection because they cause the disruption of the normal epithelial barrier by genital ulceration and/or microulceration; and by accumulation of pools of HIV-susceptible or HIV-infected cells (lymphocytes and macrophages) in semen and vaginal secretions. Epidemiological studies from sub-Saharan Africa, Europe and North America have suggested that there is approximately a four times greater risk of becoming infected with HIV in the presence of a genital ulcer such as those caused by syphilis and/or chancroid. There is also a significant though lesser increased risk in the presence of STIs such as gonorrhea, Chlamydial infection and trichomoniasis which cause local accumulations of lymphocytes and macrophages.[60]
Transmission of HIV depends on the infectiousness of the index case and the susceptibility of the uninfected partner. Infectivity seems to vary during the course of illness and is not constant between individuals. An undetectable plasma viral load does not necessarily indicate a low viral load in the seminal liquid or genital secretions. Each 10-fold increment of blood plasma HIV RNA is associated with an 81% increased rate of HIV transmission.[60][61] Women are more susceptible to HIV-1 infection due to hormonal changes, vaginal microbial ecology and physiology, and a higher prevalence of sexually transmitted diseases.[62][63] People who are infected with HIV can still be infected by other, more virulent strains.
During a sexual act, only male or female condoms can reduce the chances of infection with HIV and other STDs and the chances of becoming pregnant. The best evidence to date indicates that typical condom use reduces the risk of heterosexual HIV transmission by approximately 80% over the long-term, though the benefit is likely to be higher if condoms are used correctly on every occasion.[64] The effective use of condoms and screening of blood transfusion in North America, Western and Central Europe is credited with contributing to the low rates of AIDS in these regions. Promoting condom use, however, has often proved controversial and difficult. Many religious groups, most noticeably the Roman Catholic Church, have opposed the use of condoms on religious grounds, and have sometimes seen condom promotion as an affront to the promotion of marriage, monogamy and sexual morality. Defenders of the Catholic Church's role in AIDS and general STD prevention state that, while they may be against the use of contraception, they are strong advocates of abstinence outside marriage.[65] This attitude is also found among some health care providers and policy makers in sub-Saharan African nations, where HIV and AIDS prevalence is extremely high.[66] They also believe that the distribution and promotion of condoms is tantamount to promoting sex amongst the youth and sending the wrong message to uninfected individuals. However, no evidence has been produced that promotion of condom use increases sexual promiscuity,[67] and abstinence-only programs have been unsuccessful in the United States both in changing sexual behavior and in reducing HIV transmission.[68] Evaluations of several abstinence-only programs in the US showed a negative impact on the willingness of youths to use contraceptives, due to the emphasis on contraceptives' failure rates.[69] The male latex condom, if used correctly without oil-based lubricants, is the single most effective available technology to reduce the sexual transmission of HIV and other sexually transmitted infections. Manufacturers recommend that oil-based lubricants such as petroleum jelly, butter, and lard not be used with latex condoms, because they dissolve the latex, making the condoms porous. If necessary, manufacturers recommend using water-based lubricants. Oil-based lubricants can however be used with polyurethane condoms.[70] Latex condoms degrade over time, making them porous, which is why condoms have expiration dates. In Europe and the United States, condoms have to conform to European (EC 600) or American (D3492) standards to be considered protective against HIV transmission.
The female condom is an alternative to the male condom and is made from polyurethane, which allows it to be used in the presence of oil-based lubricants. They are larger than male condoms and have a stiffened ring-shaped opening, and are designed to be inserted into the vagina. The female condom contains an inner ring, which keeps the condom in place inside the vagina — inserting the female condom requires squeezing this ring. However, at present availability of female condoms is very low and the price remains prohibitive for many women. Preliminary studies suggest that, where female condoms are available, overall protected sexual acts increase relative to unprotected sexual acts, making them an important HIV prevention strategy.[71]
With consistent and correct use of condoms, there is a very low risk of HIV infection. Studies on couples where one partner is infected show that with consistent condom use, HIV infection rates for the uninfected partner are below 1% per year.[72]
The United States government and health organizations both endorse the ABC Approach to lower the risk of acquiring AIDS during sex:
- Abstinence or delay of sexual activity, especially for youth,
- Being faithful, especially for those in committed relationships,
- Condom use, for those who engage in risky behavior.
This approach has been very successful in Uganda, where HIV prevalence has decreased from 15% to 5%. However, more has been done than just this. As Edward Green, a Harvard medical anthropologist, put it, "Uganda has pioneered approaches towards reducing stigma, bringing discussion of sexual behavior out into the open, involving HIV-infected people in public education, persuading individuals and couples to be tested and counseled, improving the status of women, involving religious organizations, enlisting traditional healers, and much more." However, criticism of the ABC approach is widespread because a faithful partner of an unfaithful partner is at risk of contracting HIV and that discrimination against women and girls is so great that they are without voice in almost every area of their lives.[73] Other programs and initiatives promote condom use more heavily. Condom use is an integral part of the CNN Approach. This is:
- Condom use, for those who engage in risky behavior,
- Needles, use clean ones,
- Negotiating skills; negotiating safer sex with a partner and empowering women to make smart choices.
In December 2006, the last of three large, randomized trials confirmed that male circumcision lowers the risk of HIV infection among heterosexual African men by around 50%. It is expected that this intervention will be actively promoted in many of the countries worst affected by HIV, although doing so will involve confronting a number of practical, cultural and attitudinal issues. Some experts fear that a lower perception of vulnerability among circumcised men may result in more sexual risk-taking behavior, thus negating its preventive effects.[74] Furthermore, South African medical experts are concerned that the repeated use of unsterilized blades in the ritual circumcision of adolescent boys may be spreading HIV.[75]
Exposure to infected body fluids
This transmission route is particularly relevant to intravenous drug users, hemophiliacs and recipients of blood transfusions and blood products. Sharing and reusing syringes contaminated with HIV-infected blood represents a major risk for infection with not only HIV, but also hepatitis B and hepatitis C. Needle sharing is the cause of one third of all new HIV-infections and 50% of hepatitis C infections in North America, China, and Eastern Europe. The risk of being infected with HIV from a single prick with a needle that has been used on an HIV-infected person is thought to be about 1 in 150 (see table above). Post-exposure prophylaxis with anti-HIV drugs can further reduce that small risk.[76] Health care workers (nurses, laboratory workers, doctors etc) are also concerned, although more rarely. This route can affect people who give and receive tattoos and piercings. Universal precautions are frequently not followed in both sub-Saharan Africa and much of Asia because of both a shortage of supplies and inadequate training. The WHO estimates that approximately 2.5% of all HIV infections in sub-Saharan Africa are transmitted through unsafe healthcare injections.[77] Because of this, the United Nations General Assembly, supported by universal medical opinion on the matter, has urged the nations of the world to implement universal precautions to prevent HIV transmission in health care settings.[78] Drug abuse has an additional effect of an increased tendency to engage in unprotected sexual intercourse [79].
The risk of transmitting HIV to blood transfusion recipients is extremely low in developed countries where improved donor selection and HIV screening is performed. However, according to the WHO, the overwhelming majority of the world's population does not have access to safe blood and "between 5% and 10% of HIV infections worldwide are transmitted through the transfusion of infected blood and blood products".[80]
Medical workers who follow universal precautions or body-substance isolation, such as wearing latex gloves when giving injections and washing the hands frequently, can help prevent infection by HIV.
All AIDS-prevention organizations advise drug-users not to share needles and other material required to prepare and take drugs (including syringes, cotton balls, the spoons, water for diluting the drug, straws, crack pipes, etc). It is important that people use new or properly sterilized needles for each injection. Information on cleaning needles using bleach is available from health care and addiction professionals and from needle exchanges. In some developed countries, clean needles are available free in some cities, at needle exchanges or safe injection sites. Additionally, many nations have decriminalized needle possession and made it possible to buy injection equipment from pharmacists without a prescription.
Mother-to-child transmission (MTCT)
The transmission of the virus from the mother to the child can occur in utero during the last weeks of pregnancy and at childbirth. In the absence of treatment, the transmission rate between the mother to the child during pregnancy, labor and delivery is 25%. However, when the mother has access to antiretroviral therapy and gives birth by caesarean section, the rate of transmission is just 1%.[49] A number of factors influence the risk of infection, particularly the viral load of the mother at birth (the higher the load, the higher the risk). Breastfeeding increases the risk of transmission by 10–15%. This risk depends on clinical factors and may vary according to the pattern and duration of breast-feeding.
Studies have shown that antiretroviral drugs, caesarean delivery and formula feeding reduce the chance of transmission of HIV from mother to child.[81] Current recommendations state that when replacement feeding is acceptable, feasible, affordable, sustainable and safe, HIV-infected mothers should avoid breast-feeding their infant. However, if this is not the case, exclusive breast-feeding is recommended during the first months of life and discontinued as soon as possible.[5] In 2005, around 700,000 children under 15 contracted HIV, mainly through MTCT, with 630,000 of these infections occurring in Africa.[82] Of the estimated 2.3 million 1.7–3.5 million children currently living with HIV, 2 million (almost 90%) live in sub-Saharan Africa.[5]
Prevention strategies are well known in developed countries, however, recent epidemiological and behavioral studies in Europe and North America have suggested that a substantial minority of young people continue to engage in high-risk practices and that despite HIV/AIDS knowledge, young people underestimate their own risk of becoming infected with HIV.[83] However, transmission of HIV between intravenous drug users has clearly decreased, and HIV transmission by blood transfusion has become quite rare in developed countries.
Treatment
There is currently no vaccine or cure for HIV or AIDS. The only known methods of prevention are based on avoiding exposure to the virus or, failing that, an antiretroviral treatment directly after a highly significant exposure, called post-exposure prophylaxis (PEP).[76] PEP has a very demanding four week schedule of dosage. It also has very unpleasant side effects including diarrhea, malaise, nausea and fatigue.[84]
Current treatment for HIV infection consists of highly active antiretroviral therapy, or HAART.[85] This has been highly beneficial to many HIV-infected individuals since its introduction in 1996 when the protease inhibitor-based HAART initially became available.[6] Current optimal HAART options consist of combinations (or "cocktails") consisting of at least three drugs belonging to at least two types, or "classes," of anti-retroviral agents. Typical regimens consist of two nucleoside analogue reverse transcriptase inhibitors (NARTIs or NRTIs) plus either a protease inhibitor or a non-nucleoside reverse transcriptase inhibitor (NNRTI). Because HIV disease progression in children is more rapid than in adults, and laboratory parameters are less predictive of risk for disease progression, particularly for young infants, treatment recommendations are more aggressive for children than for adults.[86] In developed countries where HAART is available, doctors assess the viral load, rapidity in CD4 decline, and patient readiness while deciding when to recommend initiating treatment.[87]
HAART allows the stabilization of the patient’s symptoms and viremia, but it neither cures the patient of HIV, nor alleviates the symptoms, and high levels of HIV-1, often HAART resistant, return once treatment is stopped.[88][89] Moreover, it would take more than the lifetime of an individual to be cleared of HIV infection using HAART.[90] Despite this, many HIV-infected individuals have experienced remarkable improvements in their general health and quality of life, which has led to the plummeting of HIV-associated morbidity and mortality.[91][92][93] In the absence of HAART, progression from HIV infection to AIDS occurs at a median of between nine to ten years and the median survival time after developing AIDS is only 9.2 months.[7] HAART is thought to increase survival time by between 4 and 12 years.[94][95] This average reflects the fact that for some patients — and in many clinical cohorts this may be more than fifty percent of patients — HAART achieves far less than optimal results. This is due to a variety of reasons such as medication intolerance/side effects, prior ineffective antiretroviral therapy and infection with a drug-resistant strain of HIV. However, non-adherence and non-persistence with antiretroviral therapy is the major reason most individuals fail to get any benefit from and develop resistance to HAART.[96] The reasons for non-adherence and non-persistence with HAART are varied and overlapping. Major psychosocial issues, such as poor access to medical care, inadequate social supports, psychiatric disease and drug abuse contribute to non-adherence. The complexity of these HAART regimens, whether due to pill number, dosing frequency, meal restrictions or other issues along with side effects that create intentional non-adherence also has a weighty impact.[97][98][99] The side effects include lipodystrophy, dyslipidaemia, insulin resistance, an increase in cardiovascular risks and birth defects.[100][101]
Daily multivitamin and mineral supplements have been found to reduce HIV disease progression among men and women. This could become an important low-cost intervention provided during early HIV disease to prolong the time before antiretroviral therapy is required.[102] Some individual nutrients have also been tried.[103][104] Anti-retroviral drugs are expensive, and the majority of the world's infected individuals do not have access to medications and treatments for HIV and AIDS.[105] It has been postulated that only a vaccine can halt the pandemic because a vaccine would possibly cost less, thus being affordable for developing countries, and would not require daily treatments.[105] However, after over 20 years of research, HIV-1 remains a difficult target for a vaccine.[105]
Research to improve current treatments includes decreasing side effects of current drugs, further simplifying drug regimens to improve adherence, and determining the best sequence of regimens to manage drug resistance. A number of studies have shown that measures to prevent opportunistic infections can be beneficial when treating patients with HIV infection or AIDS. Vaccination against hepatitis A and B is advised for patients who are not infected with these viruses and are at risk of becoming infected.[106] Patients with substantial immunosuppression are also advised to receive prophylactic therapy for Pneumocystis jiroveci pneumonia (PCP), and many patients may benefit from prophylactic therapy for toxoplasmosis and Cryptococcus meningitis as well.[84]
Various forms of alternative medicine have been tried to treat symptoms or alter the course of the disease.[107] In the first decade of the epidemic when no useful conventional treatment was available, a large number of people with AIDS experimented with alternative therapies. The definition of "alternative therapies" in AIDS has changed since that time. Then, the phrase often referred to community-driven treatments, untested by government or pharmaceutical company research, that some hoped would directly suppress the virus or stimulate immunity against it. Examples of alternative medicine that people hoped would improve their symptoms or their quality of life include massage, stress management, herbal and flower remedies such as boxwood,[108][109] and acupuncture;[107] when used with conventional treatment, many now refer to these as "complementary" approaches. Despite the widespread use of complementary and alternative medicine by people living with HIV/AIDS, the effectiveness of these therapies has not been established.
Epidemiology
UNAIDS and the WHO estimate that AIDS has killed more than 25 million people since it was first recognized in 1981, making it one of the most destructive epidemics in recorded history. Despite recent, improved access to antiretroviral treatment and care in many regions of the world, the AIDS epidemic claimed an estimated 2.8 million (between 2.4 and 3.3 million) lives in 2005 of which more than half a million (570,000) were children.[5]
Globally, between 33.4 and 46 million people currently live with HIV.[5] In 2005, between 3.4 and 6.2 million people were newly infected and between 2.4 and 3.3 million people with AIDS died, an increase from 2003 and the highest number since 1981.[5]
Sub-Saharan Africa remains by far the worst affected region, with an estimated 21.6 to 27.4 million people currently living with HIV. Two million [1.5–3.0 million] of them are children younger than 15 years of age. More than 64% of all people living with HIV are in sub-Saharan Africa, as are more than three quarters (76%) of all women living with HIV. In 2005, there were 12.0 million [10.6–13.6 million] AIDS orphans living in sub-Saharan Africa 2005.[5] South & South East Asia are second worst affected with 15%. AIDS accounts for the deaths of 500,000 children in this region. Two-thirds of HIV/AIDS infections in Asia occur in India, with an estimated 5.7 million infections (estimated 3.4 – 9.4 million) (0.9% of population), surpassing South Africa's estimated 5.5 million (4.9–6.1 million) (11.9% of population) infections, making it the country with the highest number of HIV infections in the world.[111] In the 35 African nations with the highest prevalence, average life expectancy is 48.3 years— 6.5 years less than it would be without the disease.[112]
The latest evaluation report of the World Bank's Operations Evaluation Department assesses the effectiveness of the World Bank's country-level HIV/AIDS assistance, defined as policy dialogue, analytic work, and lending, with the explicit objective of reducing the scope or impact of the AIDS epidemic.[113] This is the first comprehensive evaluation of the World Bank's HIV/AIDS support to countries, from the beginning of the epidemic through mid-2004. Because the Bank's assistance is for implementation of government programs by government, it provides important insights on how national AIDS programs can be made more effective.
The development of HAART as effective therapy for HIV infection and AIDS has substantially reduced the death rate from this disease in those areas where it is widely available. This has created the misperception that the disease has gone away. In fact, as the life expectancy of persons with AIDS has increased in countries where HAART is widely used, the number of persons living with AIDS has increased substantially. In the United States, the number of persons with AIDS increased from about 35,000 in 1988 to over 220,000 in 1996.
In Africa, the number of MTCT and the prevalence of AIDS is beginning to reverse decades of steady progress in child survival. Countries such as Uganda are attempting to curb the MTCT epidemic by offering VCT (voluntary counseling and testing), PMTCT (prevention of mother-to-child transmission) and ANC (ante-natal care) services, which include the distribution of antiretroviral therapy.
Economic Impact
HIV and AIDS retard economic growth by destroying human capital. UNAIDS has predicted outcomes for sub-Saharan Africa to the year 2025. These range from a plateau and eventual decline in deaths beginning around 2012 to a catastrophic continual growth in the death rate with potentially 90 million cases of infection.[5]
Without proper nutrition, health care and medicine that is available in developed countries, large numbers of people in these countries are falling victim to AIDS. They will not only be unable to work, but will also require significant medical care. The forecast is that this will likely cause a collapse of economies and societies in the region. In some heavily infected areas, the epidemic has left behind many orphans cared for by elderly grandparents.
The increased mortality in this region will result in a smaller skilled population and labor force.[114] This smaller labor force will be predominantly young people, with reduced knowledge and work experience leading to reduced productivity. An increase in workers’ time off to look after sick family members or for sick leave will also lower productivity. Increased mortality will also weaken the mechanisms that generate human capital and investment in people, through loss of income and the death of parents.[114] By killing off mainly young adults, AIDS seriously weakens the taxable population, reducing the resources available for public expenditures such as education and health services not related to AIDS resulting in increasing pressure for the state's finances and slower growth of the economy. This results in a slower growth of the tax base, an effect that will be reinforced if there are growing expenditures on treating the sick, training (to replace sick workers), sick pay and caring for AIDS orphans. This is especially true if the sharp increase in adult mortality shifts the responsibility and blame from the family to the government in caring for these orphans.
On the level of the household, AIDS results in both the loss of income and increased spending on healthcare by the household. The income effects of this lead to spending reduction as well as a substitution effect away from education and towards healthcare and funeral spending. A study in Côte d'Ivoire showed that households with an HIV/AIDS patient spent twice as much on medical expenses as other households.
UNAIDS, WHO and the United Nations Development Programme have documented a correlation between the decreasing life expectancies and the lowering of gross national product in many African countries with prevalence rates of 10% or more. Indeed, since 1992 predictions that AIDS would slow economic growth in these countries have been published. The degree of impact depended on assumptions about the extent to which illness would be funded by savings and who would be infected.[115] Conclusions reached from models of the growth trajectories of 30 sub-Saharan economies over the period 1990–2025 were that the economic growth rates of these countries would be between 0.56 and 1.47% lower. The impact on gross domestic product (GDP) per capita was less conclusive. However, in 2000, the rate of growth of Africa's per capita GDP was in fact reduced by 0.7% per year from 1990–1997 with a further 0.3% per year lower in countries also affected by malaria.[116] The forecast now is that the growth of GDP for these countries will undergo a further reduction of between 0.5 and 2.6% per annum.[114] However, these estimates may be an underestimate, as they do not look at the effects on output per capita.[117]
Many governments in sub-Saharan Africa denied that there was a problem for years, and are only now starting to work towards solutions. Underfunding is a problem in all areas of HIV prevention when compared to even conservative estimates of the problems.
The launching of the world's first official HIV/AIDS Toolkit in Zimbabwe on October 3, 2006 is a product of collaborative work between the International Federation of Red Cross and Red Crescent Societies, World Health Organization and the Southern Africa HIV/AIDS Information Dissemination Service. It is for the strengthening of people living with HIV/AIDS and nurses by minimal external support. The package, which is in form of eight modules focusing on basic facts about HIV and AIDS, was pre-tested in Zimbabwe in March 2006 to determine its adaptability. It disposes, among other things, categorized guidelines on clinical management, education and counseling of AIDS victims at community level.[118]
The Copenhagen Consensus is a project that seeks to establish priorities for advancing global welfare using methodologies based on the theory of welfare economics. The participants are all economists, with the focus of the project being a rational prioritization based on economic analysis. The project is based on the contention that, in spite of the billions of dollars spent on global challenges by the United Nations, the governments of wealthy nations, foundations, charities, and non-governmental organizations, the money spent on problems such as malnutrition and climate change is not sufficient to meet many internationally-agreed targets. The highest priority was assigned to implementing new measures to prevent the spread of HIV and AIDS. The economists estimated that an investment of $27 billion could avert nearly 30 million new infections by 2010.
continue...
Source: Wikipedia